What is Milialar?
Milia is a non-life threatening skin condition, but can reduce quality of life for individuals affected. Milia results from dead skin cells gathering in pores and leading to painless cysts on the face that resemble pearls or grains – symptoms may include discomfort as well as aesthetic concerns that require medical evaluation from a dermatologist in order to properly diagnose and provide treatment solutions.
Genetic factors are among the primary contributors to milia, with mutations of certain genes leading to increased production of oil and death of skin cells, which in turn clogs pores and leads to the formation of these cysts. Environmental factors like sweating or using heavy skincare products that contain comedogenic ingredients may also spur its formation.
Milialar can be treated easily using topical retinoids or prescription creams that promote cell turnover and loosen keratin build-up from pores, although these medications must be used carefully not to irritate surrounding skin.
Professional extraction may be effective for severe cases; dermatologists use sterile needles or blades to break apart cysts and gently push out their contents with professional extraction, while laser therapy provides advanced solutions by targeting focused beams of light at them in order to break apart cysts and shrink their appearance; surgery may be the last resort when less conventional strategies have failed.
In this blog we are going to see about, causes, symptoms, treatment, diet and prevention of Milialar.
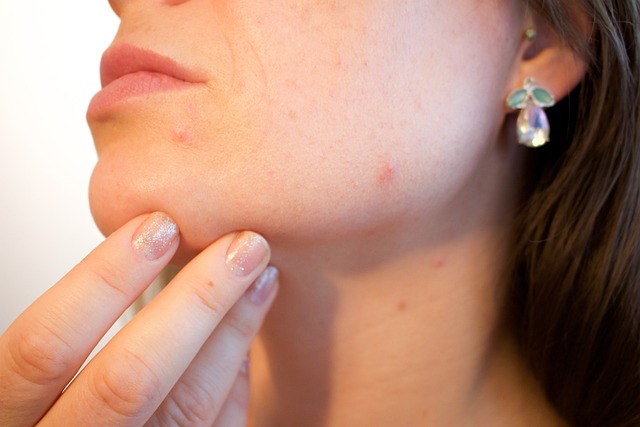
What Causes Milialar Disease?
Milia are small cysts formed when dead skin cells become trapped beneath the surface, often appearing as painless pearly white or yellow protrusions in clusters on the face (typically around eyes and cheeks) but may also occur elsewhere on the body – newborns often develop them, though most go away on their own within several weeks or months.
Other possible causes for Milialar may include excess oil that clogs pores and traps dead skin cells; hormonal fluctuations during puberty, pregnancy or menopause which cause thicker skin with more sebaceous glands to proliferate; and use of steroids creams or ointments used to treat other skin conditions like Psoriasis or Eczema. Mutations in genes which alter how fat is processed in the liver may also contribute to its formation.
While these cysts are harmless, they may be unsightly or cause discomfort. Recognizing milialar cysts early and seeking professional advice to extract or preventive measures will help alleviate symptoms while maintaining a healthier lifestyle.
Symptoms
Painless Bumps
Milialar causes the development of painless dome-shaped cysts on the skin, which appear as small bumps.
Pain, Swelling, and Itching
Milialar symptoms such as pain, swelling, and itching can make it uncomfortable, particularly when the cysts appear on sensitive areas like around the eyes and cheeks.
Redness
The skin around the milialar cysts may become red, especially after sun exposure or due to certain medications.
Itching
While milia cysts are not typically itchy like acne or pimples, they can still irritate sensitive areas, leading to occasional itching in some individuals.
Cosmetic Concerns
Milialar cysts can be cosmetically unappealing, affecting a person’s appearance.
Infection Risk
There’s a risk that milia cysts can become infected, causing additional discomfort and cosmetic concerns.
How Does It Affect Our Skin?
Your skin serves as the first line of defense against the outside world, keeping body fluids inside to avoid dehydration (dryness) and keeping harmful microbes out – without it we would get infections. Plus it contains nerve endings that allow us to detect heat, cold and pain sensation.
People living with rosacea often report that certain foods such as red wine and spicy meals aggravate their symptoms of flushing and reddening of the face, such as flushing. A dermatologist can provide guidance in selecting an effective diet tailored specifically to your condition.
Mental health is also an integral component. Stress can trigger Raynaud’s phenomenon, in which blood vessels constrict due to temperature or pressure changes and cause itchy and painful fingers and toes; depression can trigger vitiligo, which results in white patches on your skin.
Utilizing water and moisturizers are both key ways to prevent dry winter skin. Individuals suffering from itchy skin could have an underlying illness like diabetes or lymphoma that needs treating; in such instances, dermatologists may suggest other strategies for controlling itching like switching medications or applying warm compresses.
Prevention and Treatment for Milialar
There is No Cure for Milialar, But Treatment Options Can Help

Treatment
Milialar is not curable, but a dermatologist can help improve your quality of life. They can painlessly break apart and extract keratin deposits from beneath the skin.
Topical Retinoids: Topical retinoids can aid in cell turnover and loosen trapped keratin deposits from pores, which may help improve the condition.
In severe cases or complications, surgical removal by trained specialists may be necessary, but it should be done carefully to minimize scarring.
Clinical trials offer access to cutting-edge treatments not yet on the market. Participating can contribute to scientific advancement in understanding Milialar Disease.
Seek resources and support from dermatologists, family, and friends to better manage symptoms and improve your overall quality of life.
Most forms of milia typically resolve within months under proper treatment, leaving clear skin.
Prevention
Use gentle skincare measures like non-comedogenic moisturizers, sun protection, and regular exfoliation to reduce the severity of milia and prevent future outbreaks.
Milia are small cysts caused by trapped dead skin cells, unlike acne, which can be squeezed. Avoid squeezing milia to prevent scarring and infection.
Understand that primary milia result from skin damage, while secondary milia can develop due to medications, skin conditions, or hormonal fluctuations.
Milia often appear near the nose, cheeks, forehead, and chin, where sweat and oil accumulate. Excessive heat or sun exposure can worsen the condition.
To keep your skin moist, use cream and use Vitamin A serums.Take dermatologist advice.
What are the Things to Follow to Control Milialar

1 Eat a Balanced Diet
- Consider eating fruits, vegetables, whole grains, lean proteins, and healthy fats.
- Avoid sugar and processed foods in your diet.
- Regular physical activity like walking, swimming, yoga, and tai chi can help joint flexibility and reduce inflammation.
- Excess oil production, hormonal changes, and genetics can contribute to Milialar formation.
- Familial hypercholesterolemia (FH) is a genetic condition that can lead to Milialar and serious health issues.
2. Manage Stress
- Stress management through activities like meditation, mindfulness, and yoga can help control Milialar.
- Stress can worsen Milialar, impacting your quality of life.
- Topical medications and surgical removal are treatment options for Milialar.
- Effective communication involves natural gestures and body language.
- Regular exercise, such as walking and swimming, can maintain joint flexibility and strength.
3. Exercise Regularly
- Regular exercise can aid in weight loss and potentially reduce the size of Milialar cysts.
- Exercise improves overall health, boosts confidence, and relieves stress.
- It can strengthen body muscles, enhance hand-eye coordination, and promote social interaction.
- Genetic mutations, skin trauma, sweating, and heavy creams can lead to Milialar.
- Milia typically disappear on their own but may be a sign of other skin conditions.
4. Get Enough Sleep
- Aim for 7-8 hours of sleep per night to reduce Milialar symptoms.
- Listen to your body and take daytime breaks if needed.
- Milia are small, painless bumps that usually resolve without treatment.
- Consult a dermatologist if you notice Milia, as they may indicate other skin issues.
- Avoid popping or squeezing Milia, as it can lead to scarring.
5. Drink Water
- Over-the-counter retinoids can help speed up skin renewal and reduce Milia symptoms.
- Milia are small cysts caused by trapped dead skin cells beneath the skin’s surface.
- They often appear around the eyes and cheeks.
- Consult a dermatologist if you have Milia, as they can be bothersome and unsightly.
- Milia can result from genetics, sun exposure, medications, trauma, or clogged pores.
Conclusion
Milia, a non-life-threatening skin condition, results from dead skin cells accumulating in pores, forming painless cysts on the face. It can affect individuals’ quality of life but is manageable. Genetic factors, hormonal changes, and environmental factors like skincare products contribute to its formation. Treatment options include topical retinoids, surgical removal, or laser therapy. Prevention involves gentle skincare, avoiding squeezing, and understanding primary and secondary milia.
Frequently Asked Questions
1. What causes Milialar Disease?
Milialar is caused by trapped dead skin cells, excess oil production, hormonal changes, genetics, and medication use.
2. What are the symptoms of Milialar?
Symptoms include painless bumps, discomfort, swelling, itching, redness, cosmetic concerns, and infection risk.
3. How can Milialar be treated?
Treatment options include topical retinoids, surgical removal, and laser therapy, with consultation from a dermatologist.
4. What are the key preventive measures for Milialar?
Prevent Milialar with gentle skincare, no squeezing, recognizing primary and secondary milia, and skin hygiene.
5. What’s the difference between Milialar and Milia?
Milialar refers to the condition and its symptoms, while Milia are the small cysts themselves, both related to this skin issue.







